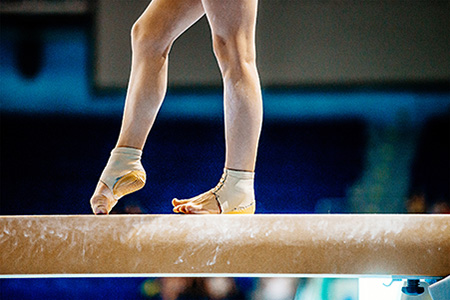As children grow, their gait, or the way they walk, develops in stages that reflect both physical and neurological maturity. It is normal for toddlers to walk with their feet wide apart or appear a bit unsteady at first. Over time, their coordination improves, and their stride becomes more fluid. However, certain patterns like frequent tripping, toe-walking, or limping may signal developmental concerns that should not be overlooked. Early identification of gait abnormalities can help prevent future discomfort or mobility challenges. A child’s foot structure, muscle tone, and even leg alignment all play a role in how they move. Paying attention to how your child walks, runs, and stands can provide early clues to potential issues that may benefit from professional guidance. If you notice irregularities in your child’s gait or foot development, it is suggested that you see a podiatrist for an exam and necessary treatment.
If you have any concerns about your feet, contact Scott Samera, DPM from Samera / Foot + Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
- Biomechanics dates back to the BC era in Egypt where evidence of professional foot care has been recorded.
- In 1974, biomechanics gained a higher profile from the studies of Merton Root, who claimed that by changing or controlling the forces between the ankle and the foot, corrections or conditions could be implemented to gain strength and coordination in the area.
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our office located in Lake City and Branford, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.